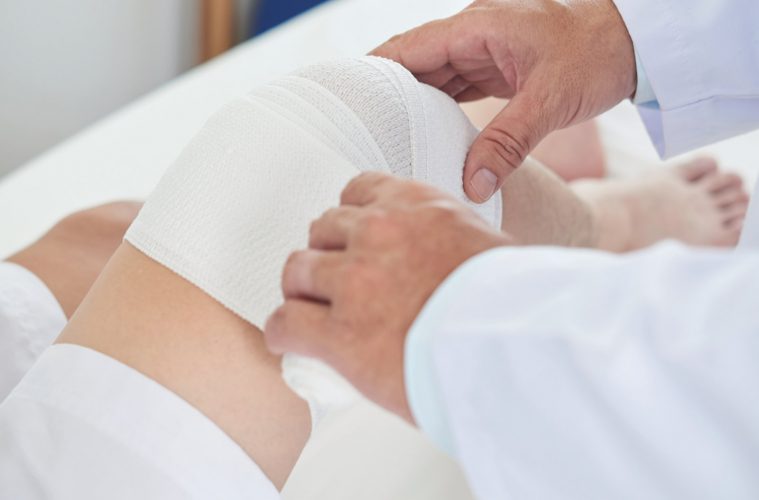
The speed of wound healing depends on the nature of the wound but also the health status of the individual. Patients with; diabetes, Raynaud’s disease, heart disease and rheumatoid arthritis have skin that is more vulnerable to damage and slower to repair and this is also true in older patients. Smoking, malnutrition and side-effects of certain medicines slow healing.
No single dressing is suitable for all stages of healing or types of wounds, so effective management depends on good product knowledge and regular assessment of the wound.
Too often patients interfere inappropriately with wounds. Routine wound cleaning is seldom necessary and wounds only need irrigation to remove debris or foreign material. Wounds tend to look after themselves. If wound cleansing is required then this is done at room temperature with sodium chloride. Cool or cold liquids will reduce the wound healing process.
Healing only proceeds efficiently at normal body temperature. Replacing dressings too frequently can be traumatic and can set back granulation and epithelial cell growth. Non-adhesive dressings are best. Certainly where there is “strike-through” – blood or exudate on external surface of the dressing – the dressing should be changed as this allows entry of infection. Antiseptics including alcohol-based agents are seldom of benefit as they interfere with the natural healing processes.
The goal of wound management is to facilitate cosmetically acceptable
healing in the shortest possible time. Additional objectives are to: remove extensive areas of necrosis, ease pain and eliminate foul odours.
Additionally, there are many types of wounds that will not heal until their underlying causes are addressed such as pressure ulcers where pressure must be relieved.
The choice of wound dressing depends on many factors but the ideal dressing; reduces wound trauma, excludes infection, ensures a moist environment and maintains normal body temperature. Specific types of wounds will need additional features. For example necrotic tissue will automatically debride from healthy tissue underneath.
However, if dead tissue is exposed to a drying atmosphere it can dehydrate and shrink to form a hard black or “olive” lump. This will delay autolysis
indefinitely and can cause pain. For necrotic wounds therefore rehydrating
the wound and removing hard, dead tissue is key.
Hydrogel dressings have 60–90% water content and draw moisture through the wound, rehydrating the dead tissue and making it easier to remove. Because they are occlusive, they may promote overgrowth of anaerobic bacteria so are contraindicated for infected wounds.
For wounds with high levels of exudate an alginate dressing may be more appropriate. Derived from seaweed, alginates can absorb large amounts of exudates yet maintain a moist wound environment.
Slough is a complex mixture of fibrin, proteins, serous exudates, leucocytes and bacteria. It can build up rapidly on the surface of previously clean wounds and become too thick to be removed by swabbing or irrigation. Slough readily supports bacterial growth so affected wounds should be properly treated to enable wound healing.
It is important not to overhydrate the wound to avoid maceration leading to further tissue breakdown. Alginates covered with either a semipermeable film dressing or a hydrocolloid dressing will maintain a moist healing environment and draw away excess exudates.
For infected wounds, systemic antibiotics are indicated in addition to an antimicrobial dressing. In all cases, a wound swab should be sent for culture and sensitivity testing. Topical antibiotics, such as mupirocin and
metronidazole, are rarely used because of concerns about microbial resistance. Antimicrobial dressings contain; iodine, silver or honey and these can be helpful to reduce bacterial load.
Granulation tissue is a fragile mixture of proteins and polysaccharides linked by collagens to create a highly vascular gel with a red appearance.
Granulating wounds must be kept warm and moist and exudates must be managed. Wound dressings are chosen depending on the type of granulation occurring for example how deep the wound is.
In the final stage of wound healing, epithelial cells advance in a sheet across the wound, starting at the wound margins before meeting in the middle. The aim for this stage of healing is to keep the wound moist until it closes.
Exercise
In this short article it has not been possible to list all dressing. For your CPD make a list of dressing you dispense and put them into the categories discussed in the article.